A Functional Guide to Brain Recovery
Bhakti Brain Health Clinic

Copyright © 2025 by Bhakti Brain Health Clinic
All rights reserved.
No portion of this book may be reproduced in any form without written permission from the publisher or author, except as permitted by U.S. copyright law.
This publication is designed to provide accurate and authoritative information in regard to the subject matter covered. It is sold with the understanding that neither the author nor the publisher is engaged in rendering legal, investment, accounting, or other professional services.
While the publisher and author have used their best efforts in preparing this book, they make no representations or warranties concerning the accuracy or completeness of the book’s contents and specifically disclaim any implied warranties of merchantability or fitness for a particular purpose.
No warranty may be created or extended by sales representatives or written sales materials. The advice and strategies contained herein may not be suitable for your situation. You should consult with a professional when appropriate.
Neither the publisher nor the author shall be liable for any loss of profit or other commercial damages, including but not limited to special, incidental, consequential, personal, or other damages.
For permissions, inquiries, or additional resources, contact:
neurofeedback@bhakticlinic.com
Copyright
Table of Contents
About The Author
Foreword
Bhakti Brain Health Clinic is a center of excellence dedicated to the functional assessment and neurophysiological treatment of brain-based conditions, including concussion and traumatic brain injury (TBI). Located at the intersection of cutting-edge neuroscience and compassionate care, the clinic offers an integrative approach that combines advanced diagnostics with customized neurotherapy interventions.
Specializing in modalities such as quantitative EEG (QEEG), event-related potentials (ERPs), neurofeedback, neurostimulation, photobiomodulation, and audiovisual entrainment, Bhakti Brain Health Clinic serves individuals seeking restoration from brain dysregulation.
The clinic is guided by the belief that true healing requires more than symptom management; it demands a deep understanding of how the brain communicates, regulates, and recovers. With a commitment to ongoing research, clinical excellence, and patient empowerment, BBHC helps clients rebuild their lives from the inside out.
This book reects the clinic’s philosophy: that the brain can heal, and that with the right tools and guidance, recovery is not only possible, it’s measurable.
Concussions and traumatic brain injuries (TBIs) affect millions of people each year: athletes, accident victims, veterans, and children alike. Yet, despite the prevalence and impact of these injuries, many individuals are left navigating a confusing maze of symptoms, appointments, and conicting advice, often without clear answers or lasting relief. The invisible nature of brain injury can compound the distress, leaving individuals not only impaired but also misunderstood.
This book is born from the conviction that healing is possible, even when the path forward isn’t obvious.
At Bhakti Brain Health Clinic, the clinical team has spent years working at the intersection of neuroscience, psychology, and integrative care, using advanced tools to assess and support brain function. Their approach does not stop at alleviating symptoms. Instead, it aims to understand and regulate the root causes of brain dysfunction, helping clients rebuild from the inside out. This functional perspective, grounded in science and guided by compassion, informs every chapter of this book.
The pages that follow are an invitation to learn, to reframe, and to hope. They offer readers a window into what’s possible when we treat the brain not as a static organ, but as a dynamic system with incredible potential for self-regulation and recovery.
Through clear explanations, real-life case studies, and insights into the science of neurotherapy, the book sheds light on how cutting-edge interventions such as QEEG, neurofeedback, neurostimulation, and photobiomodulation can help restore quality of life, even long after an injury has occurred.
Neurotherapy for Concussion and Traumatic Brain Injury
Whether you are someone living with post-concussion symptoms, a caregiver, or a clinician seeking new tools, this book is designed to support and inform you. It is a compassionate, evidence-based guide through the complexity of brain injury and a testament to the resilience of the human nervous system.
Healing is not always linear. But it is possible.
— The Team at Bhakti Brain Health Clinic
Concussions and traumatic brain injuries (TBIs) are among the most misunderstood and underdiagnosed conditions in modern healthcare. Their symptoms are often invisible, unpredictable, and deeply disruptive. While many individuals are advised to simply “rest and wait,” countless others are left to navigate a fragmented system without a clear path forward. At Bhakti Brain Health Clinic, we believe there is a better way —one that combines clinical precision with neuroplasticity.
This book evolved from a functional forum presentation given by our team, where we shared the science, tools, and real-world outcomes of our work with individuals recovering from brain injuries. We have expanded that conversation here, offering a structured and supportive guide to understanding how functional neurotherapy can illuminate, intervene, and initiate healing after concussion and TBI.
At Bhakti Brain Health Clinic, we are a multidisciplinary team of clinicians, neurofeedback technicians, and administrators dedicated to restoring brain health. Our clinic integrates functional brain assessments with neurotherapy interventions, offering both in-clinic and at-home programs.
Bhakti means “devotion,” and that principle is reected in every aspect of our care. We are devoted to clinical excellence, yes, but also to curiosity, humility, and heart. Our work stands at the intersection of rigorous data and compassionate connection.
Our approach is rooted in the understanding that the brain is not broken; it is dysregulated. By identifying where and how that dysregulation occurs, we create personalized treatment plans that guide the brain back toward balance. Every member of our team is trained not only in the technology but also in the human connection that makes healing possible. Our clients are not case numbers; they are collaborators in a journey toward recovery.
We use quantitative EEG, event-related potentials, neurofeedback, neurostimulation, photobiomodulation, and other cutting-edge methods, not because they are trendy, but because they provide measurable, lasting results when applied with precision. And, we also know that healing isn’t only about metrics; it’s about restoring agency, function, and identity.
This book is designed to be informative, expository, and above all, helpful. Whether you are recovering from a recent concussion, supporting a loved one with persistent symptoms, or working as a clinician seeking new tools, this guide is for you.
You’ll fnd:
Each chapter builds upon the last, beginning with foundational concepts and progressing to speci~c interventions and outcomes. We have aimed to strike a balance between clinical depth and accessible language, so you can both understand and apply the information provided.
Above all, this book is a message of hope. The brain can heal. And with the right support, so can you.
The Vision: Science, Compassion, and Customization
Bhakti means “devotion,” and that principle is reected in every aspect of our care. We are devoted to clinical excellence, yes, but also to curiosity, humility, and heart. Our work stands at the intersection of rigorous data and compassionate connection.
A concussion, also known as a mild traumatic brain injury (mTBI), is a disruption in normal brain function caused by an external force, usually a blow, jolt, or sudden movement of the head. It doesn’t require a loss of consciousness, external bleeding, or even a direct impact to the head. What defines a concussion is not what can be seen on the outside, but what happens on the inside of the brain, particularly how its delicate tissues stretch, twist, or become chemically imbalanced.
At its core, a concussion is a functional injury. Rather than damaging brain structures in ways that are always visible on a scan, it disturbs how neurons fire, how networks synchronize, and how the brain communicates with itself and the body. These disruptions can have cascading effects across cognitive, emotional, and physical domains.
While it is termed “mild,” the reality is that the impact on daily life can be anything but that. Many individuals struggle for months, or even years, without proper understanding, diagnosis, or care.
Despite decades of research, misconceptions about concussions persist. One of the most damaging is the idea that a concussion is simply a bump to the head that resolves with rest. In truth, concussions can have long-lasting physiological, neurological, and psychological effects, especially when unrecognized or untreated.
Common myths include:
In actual fact, most concussions do not involve loss of consciousness.
Rapid acceleration-deceleration (as in whiplash) can cause a concussion without direct impact.
Many standard imaging tools fail to detect functional changes associated with concussion.
While initial rest is important, prolonged inactivity can slow recovery if not paired with appropriate therapy.
The reality is that concussions are neurophysiological injuries, not always structural ones, and they require more than time to heal effectively.
No two concussions are exactly alike. The symptoms depend on the force, the part of the brain affected, and the individual’s pre-injury baseline. Some may experience cognitive fog, others emotional volatility, and still others physical impairments such as headaches or balance problems.
Common post-concussion symptoms include:
 Some individuals may experience just one or two of these symptoms, while others may experience many. In some cases, symptoms worsen over time or appear delayed. It’s important to note that symptoms may stem not just from the injury itself, but also from the nervous system’s dysregulated response to it.
Some individuals may experience just one or two of these symptoms, while others may experience many. In some cases, symptoms worsen over time or appear delayed. It’s important to note that symptoms may stem not just from the injury itself, but also from the nervous system’s dysregulated response to it.
This variability is one of the reasons that concussion is so often overlooked or misdiagnosed; it does not present in a predictable or uniform way.
Standard imaging techniques, such as CT scans, MRI, and even PET scans, are powerful tools, but they primarily detect anatomical abnormalities, including bleeding, swelling, or structural damage. Because concussions are often functional disruptions, not structural injuries, they may not show up at all on these scans.
This limitation leads to one of the most common frustrations for patients: being told “everything looks normal” when they continue to feel far from it.
Even when more advanced imaging like diffusion tensor imaging (DTI) or functional MRI is used, it often lacks the resolution or specificity needed to detect micro-level dysregulation in real-time.
At BBHC, this gap is addressed through functional neuroimaging, including quantitative EEG (QEEG) and event-related potentials (ERP). These tools enable clinicians to observe how the brain functions, not just what it looks like. They offer key insights into patterns of dysregulation, connectivity, and neurophysiological coherence that traditional scans cannot reveal.
In other words, where structural imaging examines the hardware, functional neuroimaging focuses on the software. And it’s the software, how the brain communicates, that so often needs repair after concussion.
Understanding a concussion or traumatic brain injury begins with asking the right question, not “What does the brain look like?” but rather, “How is the brain functioning?” Traditional diagnostic tools often fall short because they examine only structure. Functional injuries, those that affect how neurons communicate, fire, and coordinate, require a functional approach to diagnosis.
At Bhakti Brain Health Clinic, the foundation of concussion assessment lies in evaluating brain function at the level of electrical activity and neurophysiological response. This chapter outlines the key tools used in that process and why a comprehensive, data-driven model is fundamental for effective treatment planning.
 When someone sustains a head injury, medical imaging is usually the first step in care. CT scans and MRIs rule out critical structural issues such as bleeding, fractures, or swelling. These scans are key for emergency medicine, but often yield no findings in mild or moderate concussions.
When someone sustains a head injury, medical imaging is usually the first step in care. CT scans and MRIs rule out critical structural issues such as bleeding, fractures, or swelling. These scans are key for emergency medicine, but often yield no findings in mild or moderate concussions.
That’s because concussions rarely cause the type of gross anatomical damage these tools are designed to detect. The issue lies not in the hardware of the brain, but in the communication networks; the speed, timing, and coherence of electrical signaling between brain regions.
This is where functional neuroimaging becomes indispensable. At BBHC, two primary tools are used to map and evaluate these disruptions: Quantitative EEG (QEEG) and Event-Related Potentials (ERP).
QEEG is the process of measuring and analyzing brainwave activity across multiple regions of the brain. While a traditional EEG is useful for identifying seizures or overt abnormalities, QEEG allows clinicians to compare a client’s brainwave patterns to a normative database of healthy individuals. This comparison reveals areas of excess activity, deficiency, or dysregulation.
Key features of QEEG:
One of the most striking QEEG findings seen in individuals with concussion is what’s colloquially referred to as “Blue Brain”, an EEG pattern marked by low- voltage, under-functioning neural networks. Other patterns include excess slow- wave activity (delta and theta) or spindling fast-wave activity (beta) in localized areas, all of which can point to disruption following injury.
While QEEG doesn’t “diagnose” concussion in a binary way, it provides a powerful map of the terrain, revealing the where, what, and how of brain dysfunction.
ERP testing measures the brain’s electrical response to specific stimuli, such as sights, sounds, or cognitive tasks. While QEEG shows the brain at rest, ERP examines the brain in action. It measures how quickly and efficiently the brain processes information and responds to events in real-time.
Benefits of ERP:
When used together, QEEG and ERP offer a dynamic picture of brain function. One shows the terrain; the other reveals how well traffic is moving through it.
While QEEG and ERP are invaluable tools, they are not without limits. EEG cannot definitively prove that a concussion caused an abnormality; it can only suggest dysregulation that aligns with known patterns of post-concussive brain injury.
Strengths:
Limitations:
For this reason, BBHC emphasizes a multi-domain model, combining EEG data with client history, symptom profiles, behavioral measures, and, in some cases, genetic or metabolic testing.
Effective concussion care does not rely on a single tool. Instead, it draws on a network of information, from the client’s lived experience to their physiological markers, to form a coherent and actionable understanding of the injury.
At BBHC, each assessment is:
This approach moves beyond guesswork and symptom chasing. It creates a roadmap for functional recovery, giving clinicians and clients alike the confidence that they are working with the brain, not just the behavior.
Curious about your brain’s electrical patterns? Schedule a QEEG and ERP evaluation to get a personalized map of your brain’s function.
A concussion may be labeled “mild,” but its effects can trigger profound changes at the cellular and systemic level of the brain. These changes are not usually visible on a scan, nor are they always immediate. In many cases, symptoms develop over days, weeks, or even months, driven by a cascade of biochemical disruptions, energetic deficits, and neuroinflammatory processes. These impair the brain’s ability to function and regulate itself.
Understanding the physiology of injury allows clinicians to not only explain symptoms but also target them at the source. Let’s explore what happens inside the brain after a concussion and introduce key concepts that guide treatment decisions in a functional neurotherapy model.
When the brain experiences sudden acceleration or impact, it responds with more than just mechanical motion. An electrochemical shockwave disrupts the delicate balance of ions and neurotransmitters required for normal brain function.
Sodium-Potassium Pump Disruption
The sodium-potassium pump is a cellular mechanism responsible for maintaining the electrical stability of neurons. It moves sodium ions out of the cell and potassium ions into the cell, allowing neurons to reset after firing and prepare for the next signal.
After a concussion, this pump becomes disrupted due to mechanical strain and sudden depolarization. The result is an imbalance in electrical gradients, leaving neurons either hyper-excitable (firing too easily) or hypo-responsive (not firing at all). This alone can affect cognitive clarity, attention, and emotional regulation.
Calcium, Glutamate, and Mitochondrial Dysfunction
A key effect of concussion is the excessive release of glutamate, a primary excitatory neurotransmitter. When glutamate floods the brain, it causes overactivation of neurons and an influx of calcium ions into cells.
This calcium overload damages mitochondria, the cell’s energy producers, disrupting their ability to generate adenosine triphosphate (ATP), the energy currency of the brain. Mitochondrial dysfunction weakens the brain’s capacity for self-repair and slows down every process from neural firing to waste clearance.
The result is a brain running low on fuel and overloaded with demand, a recipe for chronic symptoms and delayed recovery.
Oxygen and Glucose Deficits, ATP Failure
Following the disruption of the sodium-potassium pump and mitochondrial activity, the brain enters a state of energy crisis. Oxygen and glucose metabolism decline, ATP production falters, and neurons begin to operate in survival mode.
This energetic shortfall can last for days or even weeks, depending on the severity of the injury and the individual’s baseline resilience. During this time, the brain is vulnerable to secondary insults; even mild exertion or emotional stress can exacerbate symptoms.
Left unaddressed, this deficit can evolve into a chronic low-energy state, contributing to long-term fatigue, cognitive sluggishness, and impaired motivation.
Neuroinflammation and Chronic Dysregulation
In parallel to the metabolic cascade, concussion often triggers a prolonged neuroinflammatory response. As the brain detects injury, it sends immune cells to the affected areas to contain damage and initiate repair. In an ideal scenario, this inflammation is short-lived and resolves on its own.
In many individuals, the inflammation often becomes chronic. This can result from repeated injuries, inadequate healing, or disruptions in the brain’s immune regulation. Neuroinflammation is known to interfere with neurotransmission, promote cellular toxicity, and prolong symptoms of depression, anxiety, and cognitive decline.
Inflammation can generate false signals of continued danger in the nervous system, locking the brain into patterns of hypervigilance, dysregulation, or shutdown. From a clinical standpoint, this shows up as mood instability, impaired sleep, sensory sensitivity, and a delayed or blunted response to therapeutic interventions.
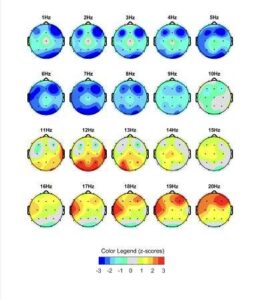 One of the most common functional brain patterns seen in post-concussion assessments is informally known as “Blue Brain.”
One of the most common functional brain patterns seen in post-concussion assessments is informally known as “Blue Brain.”
In quantitative EEG (QEEG) maps, this term refers to widespread regions of low voltage, which are visually depicted in cool tones (blue and green) that contrast with the normative average. A “blue” map usually indicates a generalized suppression of neural activity, often associated with poor signal strength, low metabolic energy, or disrupted connectivity.
This is not a diagnosis, but a functional fingerprint —a marker of how the brain is operating beneath the surface.
Blue Brain may manifest in symptoms such as:
It’s important to note that not all individuals with TBI will present with this pattern, and not all Blue Brain findings are directly attributable to the injury. However, in the context of a concussion history, Blue Brain often correlates with clinical impairment and helps guide the focus of neurofeedback and neuromodulation protocols.
The takeaway is clear: concussion is not a singular event, but a cascading system failure that affects electrical, chemical, and metabolic systems in the brain. Recognizing and addressing this complexity is what allows true healing to begin.
Once a concussion has triggered dysfunction in the brain’s electrical and biochemical systems, healing requires more than time; it requires targeted intervention. The challenge is that traditional treatments for concussion often focus on symptom management alone: medications for headaches, rest for fatigue, or therapy for mood disruption.
While those interventions can play a role, they don’t always address the underlying dysregulation in the brain’s networks. At Bhakti Brain Health Clinic the goal is not just to reduce symptoms, but to help the brain reorganize itself, reestablish balance, restore energy ow, and improve communication betwee regions. This is where neurotherapy comes in.
This chapter outlines the core tools used at BBHC to support concussion and recovery. These interventions are safe, non-invasive, and evidence-informed, designed to help the brain not only function, but thrive.
Neurofeedback is a brain training technique rooted in operant conditioning. It involves monitoring the brain’s real-time electrical activity (via EEG) and providing instant feedback to encourage more ef~cient patterns.
Here’s how it works:
Neurofeedback is especially helpful for:
Each protocol is customized based on QEEG data and symptom p making sure that the training aligns with the individual’s unique b goals.
 While neurofeedback trains the brain through learning, neurostimulation enhances physiological function directly. Techniques like transcranial electrical stimulation (tES) and pulsed electromagnetic ~eld stimulation (PEMF) deliver mild, non-invasive pulses to speci~c brain regions to improve:
While neurofeedback trains the brain through learning, neurostimulation enhances physiological function directly. Techniques like transcranial electrical stimulation (tES) and pulsed electromagnetic ~eld stimulation (PEMF) deliver mild, non-invasive pulses to speci~c brain regions to improve:
When the brain produces desired patterns (e.g., increased focus, wave activity), the feedback rewards that pattern by making the clearly or the sound becomes more audible.
Over time, the brain learns to repeat those healthier patterns on
Neurostimulation is particularly effective for:
These methods are painless and well-tolerated, and when applied systematically, they provide a physiological foundation upon which other therapies can build.
Photobiomodulation (PBM), also known as infrared light therapy, uses spe wavelengths of near-infrared light to penetrate the skull and inuence cell function in the brain. This light is absorbed by cytochrome c oxidase, an en in the mitochondria that plays a key role in energy production.
When stimulated by light, the mitochondria increase ATP output, reduce oxidative stress, and enhance cell-to-cell signaling, all of which are disrup concussion.
PBM has been shown to:
Because it is non-pharmaceutical and has minimal side effects, PBM is a powerful adjunct for clients with lingering symptoms, chronic fatigue, or m changes following a TBI.
 Audio-Visual Entrainment (AVE) is a technique that uses rhythmic pulses of light and sound to guide the brain into more regulated brainwave states.
Audio-Visual Entrainment (AVE) is a technique that uses rhythmic pulses of light and sound to guide the brain into more regulated brainwave states.
Unlike neurofeedback, which trains the brain through feedback, AVE entrains it, inviting the brain to synchronize with external frequencies.
During a session, the client wears special goggles and headphones that deliver:
AVE can help:
It is bene~cial as a daily at-home protocol, and often serves as a bridge between formal sessions in the clinic.
While some interventions require clinical supervision (like QEEG-guided neurofeedback or certain forms of neurostimulation), many clients at BBHC also use home-based tools to reinforce and extend their treatment.
Home-use options may include:
These tools provide exibility, conti which can be fundamental for those
However, at-home use is most effec guidance. BBHC clinicians tailor pro adjustments as the brain heals, mak effective.
Every brain injury is unique. The mechanisms may be similar: rotational force, metabolic cascade, and inflammation, but the human experience is deeply individual. One of the most powerful aspects of functional neurotherapy is its ability to tailor its approach to the specific needs of each individual and their unique story.
At Bhakti Brain Health Clinic, progress is measured not only by brain maps and metrics, but also by the return of agency, vitality, and selfhood. This chapter presents four real-world case studies drawn from clinical practice, each illustrating how dysregulation presents and how targeted neurotherapy can foster meaningful transformation.
This client arrived at the clinic with a long-standing history of chronic depression. Despite decades of standard care, medications, psychotherapy, and various interventions, she had not found lasting relief. She approached BBHC as a last resort, hoping for even modest improvement.
Her QEEG showed a classic “Blue Brain” pattern: widespread low voltage across multiple regions, indicating systemic underactivation. A statistical analysis of her brain activity suggested a 99.9% likelihood of traumatic brain injury, although she had no reported history of TBI.
Only after deeper inquiry did a forgotten incident emerge: a fall while skating in her youth that had resulted in hospitalization. No one at the time had labeled it a concussion, but the correlation with her depression onset was clear.
Treatment involved:
Despite initial skepticism, significant physiological and psychological changes emerged after several sessions:
As her autonomic regulation improved, so did her emotional state. She became more social, resumed exercise and cooking, and began experiencing herself as “motivated” for the first time in years. The return of function and vitality was both measurable and deeply meaningful.
This young man had sustained severe head trauma at age 13 after going over his bicycle handlebars and landing on his face. He endured extensive facial fractures, lost teeth, and underwent reconstructive surgery. Over the following years, he withdrew completely from life, spending most of his time in a dark room playing video games.
His parents had taken him around the world for treatment, trying every option available: orthopedic, psychological, neurological. Nothing had shifted the trajectory. He presented at BBHC in his late teens, largely non-verbal and emotionally flat.
Over the course of nearly 80 neurofeedback sessions, slow but profound changes began to emerge:
As neurophysiological coherence increased, his life began to undergo a transformation. He secured a job, began traveling, reconnected with his peers, and rediscovered his passion for painting. His artwork, both before and after treatment, showed a clear shift in emotional depth and complexity.
His brain map had shown excess slow-wave activity (delta and theta) and widespread dysrhythmia, classic concussion markers. Over time, those patterns shifted toward greater symmetry and regulation.
This client was a 40-year-old mother and working professional, referred to BBHC one and a half years after a motor vehicle accident resulted in a traumatic brain injury. Despite previous therapies, she continued to experience:
Her QEEG showed lateralized slow-wave activity in the temporal lobes, excess fast beta spindling, and a cycling pattern of wakefulness and stage-one sleep, suggesting persistent dysregulation. Treatment included:
Over approximately 40 sessions, she began to notice:
Most importantly, she reported a growing sense of returning to herself: “I feel like me again.” Her parenting improved, her work capacity increased, and her sense of internal order was restored.
This young client came to BBHC with a complex history of emotional dysregulation, anxiety, and executive dysfunction. She had recently sustained a concussion from a soccer injury, and over the course of training, she suffered two additional concussions, each formally diagnosed.
She had long-standing challenges even prior to the concussions, but these injuries appeared to significantly exacerbate her symptoms, including:
Her QEEG revealed “Blue Brain” patterns, excess slow activity, and elevated gamma in the insula, likely contributing to both emotional volatility and sensory overwhelm.
Her care plan included:
Her parents, who tracked her progress closely, reported significant improvements within weeks:
By the end of her initial treatment cycle, her mother shared: “She can be her true self now. It seems to be nothing short of a miracle.”
 These case studies are more than anecdotes; they are evidence of what’s possible when brain-based dysregulation is treated at its source. While recovery is rarely linear, it is achievable, even when hope feels distant.
These case studies are more than anecdotes; they are evidence of what’s possible when brain-based dysregulation is treated at its source. While recovery is rarely linear, it is achievable, even when hope feels distant.
Your story isn’t over. If you see yourself, or a loved one, in these stories, know that change is possible. Contact Bhakti Brain Health Clinic to begin a new chapter in your healing journey.
Recovery from a concussion or traumatic brain injury often defies easy measurement. It is not a simple matter of symptoms vanishing overnight, nor does it always follow a predictable path. At Bhakti Brain Health Clinic, change is understood as a process of regulation, one in which the brain reestablishes coherent rhythms, energy flow, and internal communication.
This chapter explores how healing is observed not only through subjective improvement, but through objective neurophysiological markers and profound life changes reported by clients and their families.
At the foundation of BBHC’s approach is the idea that what the client feels and what the brain shows are interconnected. Neurotherapy provides tools to track both.
QEEG (Quantitative EEG): Clients often begin with dysregulated brainwave patterns, such as excess slow-wave activity, spindling fast waves, or suppressed voltage (“Blue Brain”). As treatment progresses, these patterns shift toward normalization. Over time, coherence improves, and regional overactivation or underactivation resolves.
HRV (Heart Rate Variability): A critical marker of autonomic nervous system regulation, HRV reflects the body’s ability to adapt to stress. In post-TBI clients, HRV may appear erratic, with high variability that is disconnected from breath rhythms. With training, HRV patterns become more stable, predictable, and synchronized with respiratory cycles, indicating restored homeostasis.
Peripheral Metrics: Skin temperature, blood volume pulse, and respiratory patterns all offer insights into nervous system stability. Improvements in these markers indicate a resilient and responsive system, one that is no longer stuck in a state of chronic stress or shutdown.
These metrics provide real-time feedback during sessions, but more importantly, they validate the underlying shifts that clients experience in their daily lives.
What do these physiological changes feel like?
Clients often describe:
These shifts are significant when the injury has disrupted one’s sense of identity. As seen in the case of the professional woman recovering from a motor vehicle accident, regaining cognitive clarity and emotional stability led to a reclamation of self, both at work and at home.
For others, like the adolescent boy who had withdrawn after facial trauma, personality changes were the first sign of progress. Where there had once been silence, eye contact, and humor returned. His journey was not just one of symptom relief; it was one of reconnection.
The voice of clients and their loved ones often says more than data ever could. Here are a few reflections drawn directly from the clinic’s work:
Each of these stories highlights a key principle: the return of regulation often reveals what injury had obscured: the full range of human expression, connection, and possibility.
Too often, TBI care focuses on symptom suppression rather than functional restoration. As these stories and outcomes reveal, neurotherapy offers more than temporary relief. It supports the brain’s innate ability to:
At BBHC, healing is not defined by whether a person can “manage” their symptoms. It is measured by their capacity to engage with life: to think clearly, feel deeply, connect authentically, and act with purpose.
Whether the injury occurred months ago or decades in the past, the nervous system retains its capacity for plasticity. And with the right tools and support, recovery can be far more than functional; it can be transformational.
Healing from a brain injury requires more than a general approach. It demands a clear, personalized plan, one that honors the individuality of the injury and the person behind it. At Bhakti Brain Health Clinic, the treatment journey is guided by a structured yet flexible process designed to assess function, identify targets, and support recovery through regulation.
This chapter outlines the clinical process from intake to implementation, detailing what clients can expect and what they need to succeed.
The foundation of the Bhakti protocol is clarity through comprehensive assessment. Whether a client arrives with a recent concussion or lingering symptoms from an injury years prior, the first step is always to map the brain’s function and listen to the client’s lived experience.
The intake process includes:
This multidimensional approach makes sure that the treatment plan is based on objective data, observed behavior, and client priorities.
The QEEG provides a snapshot of functional brain patterns, highlighting underactive regions, dysregulated networks, or “Blue Brain” patterns. The ERP measures timing, processing speed, and how the brain responds to input, offering a dynamic view of cognitive performance.
These tools, combined with clinical insight, form the basis of a thorough report of findings, a document that can exceed 200 pages, rich in visual maps and neurophysiological insights.
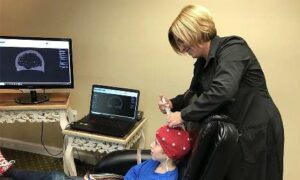 Once the assessment is complete, the team designs a custom treatment plan. No two protocols are the same; plans are tailored to match the individual’s unique brain patterns, goals, and life context.
Once the assessment is complete, the team designs a custom treatment plan. No two protocols are the same; plans are tailored to match the individual’s unique brain patterns, goals, and life context.
Key elements of the plan include:
Pacing is adjusted based on client responsiveness. Some clients benefit from intensive work over a short period; others progress more steadily over time.
The care plan is collaborative and adaptive. Progress is continually monitored through clinical observation, follow-up assessments, and feedback from the client and their support system.
Each session at BBHC is structured yet responsive to individual needs. A standard in-clinic neurotherapy session may include:
Sessions typically last between 45 and 75 minutes, depending on the therapies being used. For clients using at-home tools like audiovisual entrainment or infrared helmets, guidance is provided to aid safe and effective implementation.
Clients are never passive recipients. Each session is an interactive process, rooted in learning and adaptation. Over time, as the brain begins to self-regulate more effectively, the client’s awareness of change deepens.
Concussion recovery is not a quick fix, but with consistency, it is a highly achievable goal. Clients who succeed in neurotherapy often share several characteristics:
 Clients are reminded: Your brain is capable of change even if the injury was years ago. Even if other treatments didn’t work. The path forward isn’t about perfection—it’s about progress and regulation, guided by real data and compassionate care.
Clients are reminded: Your brain is capable of change even if the injury was years ago. Even if other treatments didn’t work. The path forward isn’t about perfection—it’s about progress and regulation, guided by real data and compassionate care.
For too long, individuals recovering from concussion and traumatic brain injury have been left without clear answers, or worse, without hope. They’ve been told their symptoms are “in their head,” that “time will heal,” or that “nothing more can be done.” These messages often stem not from malice, but from a medical model that lacks the tools to see what’s truly happening inside the injured brain.
At Bhakti Brain Health Clinic, the message is different:
The brain can heal. Dysregulation can be reversed. Recovery is possible.
This book has introduced the foundations of functional neurotherapy, a clinical approach that goes beyond symptoms to restore the rhythms, energy, and connectivity that the brain relies on to thrive. From QEEG and ERP diagnostics to neurofeedback, neurostimulation, and light-based therapies, the tools now exist to observe brain function in real-time and intervene with precision.
Tools alone are not enough. Healing requires more than technology. It needs compassionate, personalized care, grounded in science yet focused on individuals. The BBHC approach centers not only on the injury, but also on the individual, their story, and their capacity to recover.
In a world where the effects of brain injury are becoming more visible, from sports concussions to long COVID neurological symptoms, the need for functional brain care is urgent and growing. Conventional models often fall short, offering either medication without understanding or wait-and-see approaches that delay intervention.
Neurotherapy matters because:
Whether working with a child who can finally sleep, an adult who can return to work, or a client reconnecting with their sense of self, neurotherapy brings real transformation to real lives.
If you or someone you love is living with the lingering effects of a concussion or brain injury, whether recent or decades old, know this:
You are not broken. You are dysregulated. And regulation can be restored.
BBHC is here to help. Whether you are seeking a comprehensive assessment, looking for targeted support, or simply exploring new options, we invite you to reach out.
To learn more or begin your healing journey:
Visit our website at https://bhakticlinic.com/ Contact our clinic for a consultation or referral Follow our work through webinars, events, and future publications.
The nervous system is capable of extraordinary repair. With guidance, data, and care, your brain can rediscover its rhythm, and you can reclaim your life.
Every recovery starts with a roadmap. Schedule an intake appointment today and discover how a personalized, data-driven care plan can move you from dysregulation to thriving.
Audio-Visual Entrainment (AVE)
A therapeutic technique using rhythmic pulses of light and sound to guide brainwave activity into regulated states. Often used to promote relaxation, attention, and mood regulation.
Autonomic Nervous System (ANS)
The part of the nervous system responsible for involuntary body functions such as heart rate, breathing, and digestion. Includes the sympathetic (“fight or flight”) and parasympathetic (“rest and digest”) branches.
ATP (Adenosine Triphosphate)
The energy-carrying molecule in cells. Brain injuries often result in ATP depletion, contributing to fatigue and impaired function due to mitochondrial dysfunction.
Blue Brain
An informal term used to describe a QEEG map showing widespread low-voltage activity. Appears as blue or green hues on the scan and typically reflects underactivation and systemic dysregulation.
Cognitive Fog (Brain Fog)
A symptom of brain injury characterized by slowed thinking, poor concentration, and mental cloudiness. Frequently reported by individuals with post-concussion syndrome.
Coherence
In brainwave analysis, coherence refers to the level of synchronization between different brain regions. Improved coherence suggests more efficient communication and functional integration.
Event-Related Potentials (ERP)
A neurophysiological test measuring the brain’s electrical response to stimuli. It tracks speed (latency) and strength (amplitude) of cognitive processing and is used to assess attention and executive function.
Heart Rate Variability (HRV)
The variation in time between heartbeats. HRV reflects the adaptability of the autonomic nervous system and is used as a measure of stress, resilience, and nervous system regulation.
Mitochondrial Dysfunction
Impaired energy production in the brain’s cells, often caused by excess calcium influx after concussion. Leads to reduced ATP output and is associated with fatigue and cognitive slowing.
Neurofeedback
A form of biofeedback that trains the brain to regulate itself by reinforcing desired brainwave activity. Used to support attention, mood, sleep, and cognitive performance.
Neuroinflammation
Inflammatory response in the brain triggered by injury or immune dysregulation. Chronic neuroinflammation is linked to prolonged symptoms and mood disorders after TBI.
Neuroplasticity
The brain’s ability to reorganize and adapt by forming new neural connections. Functional neurotherapy leverages neuroplasticity to support recovery after concussion.
Neurostimulation
The use of mild electrical or electromagnetic signals to stimulate targeted brain regions. Helps enhance brain activity, improve blood flow, and reduce inflammation.
Photobiomodulation (PBM)
A therapy that uses red or near-infrared light to stimulate cellular energy production, reduce inflammation, and support healing in the brain post-injury.
Pulsed Electromagnetic Field (PEMF)
A non-invasive stimulation technique that uses electromagnetic fields to influence cellular activity, blood flow, and inflammation regulation.
Quantitative EEG (QEEG)
A type of brain mapping that analyzes electrical activity and compares it to normative databases. Used to identify patterns of dysregulation in individuals with concussion or TBI.
Sodium-Potassium Pump
A cellular mechanism that maintains the electrical balance across neurons. Disrupted after concussion, leading to impaired signaling and energy imbalance.
Spindling Beta
A pattern of high-frequency brainwave bursts often observed on QEEG. It can indicate overcompensation, hypervigilance, or instability in brain activity following injury.
Neurotherapy for Concussion and Traumatic Brain Injury explores innovative, data-driven treatments for brain injuries, blending cutting-edge techniques like neurofeedback, neurostimulation, and photobiomodulation with compassionate care. This comprehensive guide emphasizes the importance of addressing underlying brain dysfunction rather than just managing symptoms, offering hope for real, measurable recovery. Through compelling case studies, learn how clients have transformed their lives, reclaiming cognitive clarity and emotional stability after injury.